Amongst many perceived failures and heavy criticism, the UK has triumphed in one area of the coronavirus pandemic: its rapid vaccination program.
The UK was one of the countries which seemed to have fared the worst in the pandemic. It had one of the highest numbers of recorded cases and deaths. However, the vaccine and its rollout program are appearing to be welcome salvation and a turning point for the UK.
The vaccine program has now entered the second part of its first phase. Everyone in the top four priority groups was offered a jab by mid-February and it is now being extended to include those aged 60 and above and those with underlying health conditions.
As of Monday, 1st March, fewer than 10 patients over 80 were being sent to ICU a day, meaning that one dose of vaccine cuts the risk of hospitalization for this age bracket by more than 80%.
The hope, for the UK government, is that every adult will have been offered a vaccine by the end of July.
The question is how did the UK manage to be so successful in this area? What did the UK do differently?
Early Days:
The key to the UK’s success against other countries lies in the early days of contract making for the vaccine. The UK had a head start and it is still enjoying the fruits of its strategic negotiations.
The UK became the first country in the world to approve a COVID-19 vaccine for emergency use in early December 2020, but the Department of Health and Social Care is reported to have begun the process of planning a mass vaccination program before the first COVID-19 case in the UK had been confirmed.
Initially, the University of Oxford had planned to partner with US company Merck in the development of the vaccine. They negotiated a deal that would allow the US company to manufacture and distribute the vaccine it was in the process of developing. However, Matt Hancock, Secretary of State for Health, refused to approve the deal because it did not include any provisions which guaranteed that the vaccine would be supplied to the UK first. The British government wanted written guarantees of supply from Merck, but the company only agreed verbally. The deal fell through.
The anglo-Swedish firm, AstraZeneca, was the next chosen partner for the University of Oxford. AstraZeneca was signed on the 30th of April. Two weeks later, an agreement that 100 million doses of the vaccine would be distributed to the UK was also signed.
A separate deal securing access to 30 million doses of the Pfizer-BioNTech vaccine was announced the next month. This was increased to 40 million doses in October.
On Tuesday, the UK government said that it would receive a further 10 million doses of the COVID-19 AstraZeneca vaccine from India’s Serum Institute.
There is no doubt that the UK is leading the inoculation due to its speedy negotiations and early deals.
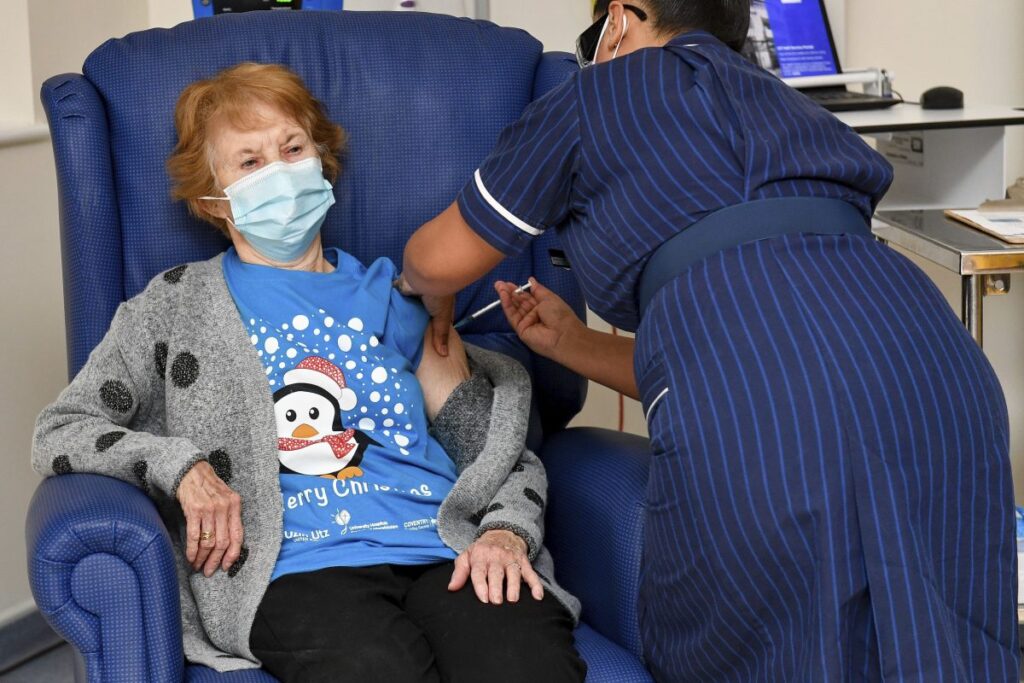
The Rollout:
At 6:31 AM on the 8th December 2020, Margaret Keenan, a UK grandmother became the first person in the world to be given the Pfizer vaccine. At the time of writing, almost 20.5 million people have received their first dose, with 845,000 people fully vaccinated.
According to the government, 98% of the country lives within a 10-mile radius of at least one vaccination center. The locations of the centers were a result of calculations made by military specialists to ensure that the promise of the ten-mile radius made by ministers was kept. Vaccines are currently being administered at over 1,500 sites across the country including mosques and museums to rugby grounds and cathedrals.
But does it work?
Some question the efficacy of the vaccines, based solely on the speed at which they were produced and rolled out. However, figures show that a single dose of the Oxford/AstraZeneca vaccine can prevent two-thirds of COVID-19 transmission.
On Wednesday, British scientists urged European countries with a slower vaccination rollout program to take note of the “remarkable” effectiveness of a single dose of Pfizer’s or AstraZeneca’s COVID-19 vaccines in frail and elderly people.

According to a study by AvonCAP, a surveillance project funded by Pfizer, a single dose of the Pfizer-BioNTech jab was 71.4% effective from 14 days at preventing hospitalization among patients with a median age of 87 years. On top of this, a single dose of the AstraZeneca vaccine was 80.4% effective by the same measures among patients with an average age of 88.
In an oral statement, Matt Hancock has hailed the vaccination program as a “national success story.” This is due to both the efficacy of the vaccines and the speed at which the country is being inoculated.
To keep up with the latest commercial news, click on commercial to get your daily dose.
Donate & Support